Not just deep breathing.
Science-informed practice.
The breathing patterns in Respirix are informed by decades of cardiovascular, autonomic, and biofeedback research. Here is a summary of the published evidence behind each protocol.
What the research shows
Four decades of peer-reviewed research behind four protocols.
Slow breathing and vagal activity
Research associates breathing at 4.5–6 breaths per minute with increased parasympathetic activity, reflected by higher RMSSD and HF-HRV.
Shaffer & Ginsberg, 2017; Zaccaro et al., 2018; Russo et al., 2017
Resonance breathing and heart rhythm variability
At ~0.1 Hz (~5.5 breaths/min), studies show heart rhythm oscillations can synchronize with the baroreflex, producing larger HRV amplitude.
Lehrer et al., 2000; Vaschillo et al., 2006; Bernardi et al., 2002
HRV biofeedback and autonomic regulation
Published research has associated HRV-guided breathing practice with changes in baroreflex sensitivity and vagal-cardiac coupling over weeks of consistent use.
Goessl et al., 2017; Lehrer & Gevirtz, 2014; Thayer & Lane, 2000
Diaphragmatic breathing with breath retention
Research suggests slow diaphragmatic breathing with controlled pauses may support autonomic balance and respiratory control.
Russo et al., 2017; Zaccaro et al., 2018
Areas of research
The published literature associates slow, paced breathing with changes in these physiological markers.
Four research-informed protocols
Each is based on a distinct body of published research.
Resonance Frequency Breathing
Studied for HRV amplitude and baroreflex engagement
Reported in studies
- Increased RMSSD and HF-HRV
- Increased HRV total power
- Changes in baroreflex sensitivity
Extended-Exhale Breathing
Studied for parasympathetic activation via prolonged exhalation
Reported in studies
- Increased vagal efferent output
- Indicators of reduced sympathetic activation
Slow Diaphragmatic Nasal Breathing
Studied for autonomic balance with gentle breath holds
Reported in studies
- Enhanced respiratory sinus arrhythmia
- Shift toward parasympathetic dominance
HRV Biofeedback Breathing
Studied for sustained HRV changes with real-time feedback
Reported in studies
- Changes in baroreflex sensitivity
- Changes in vagal-cardiac coupling
Designed for practice
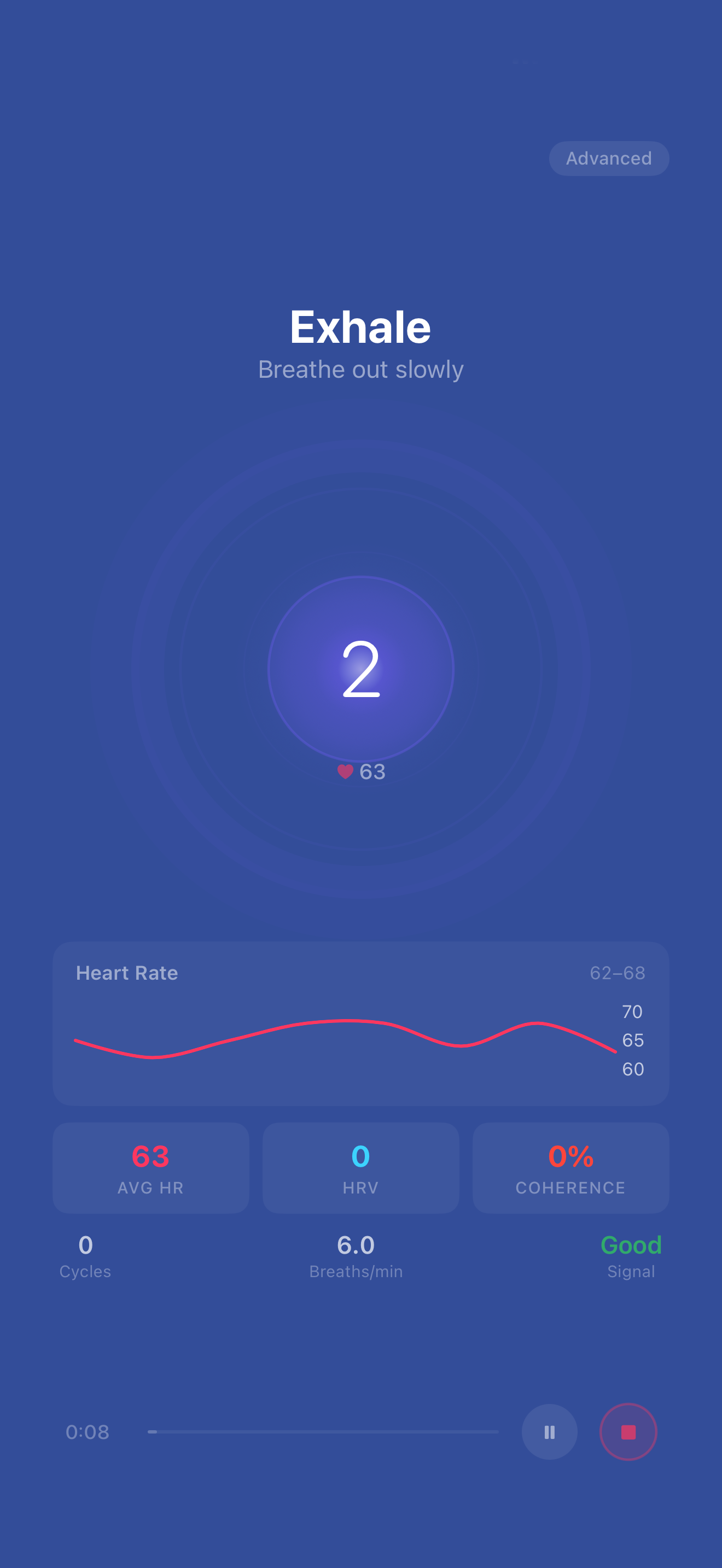
Voice cues, a visual pacer, and optional real-time HRV coherence feedback. Put your phone down and let the app guide you through each protocol.
- Follow research-informed breathing patterns
- Track HRV metrics over time
- Optional real-time coherence feedback
- Review session data to observe your own trends
What we measure
HRV metrics tracked during every session.
Primary vagal tone marker. Root mean square of successive RR interval differences. Higher values indicate stronger parasympathetic activity.
Spectral peak power at breathing frequency (~0.1 Hz) relative to total autonomic power. Indicates how well your heart rhythm synchronizes with your breath.
Beat-to-beat heart rate from BLE chest strap. Track real-time response to each breathing phase.
Continuous monitoring of RR interval validity and packet loss helps ensure your HRV data is reliable.
Why chest straps over camera PPG
For HRV biofeedback, measurement accuracy matters. Here's why Respirix uses chest-strap data.
True beat-to-beat timing
Chest straps detect the heart's electrical signal (ECG) and transmit individual RR intervals with millisecond precision. Camera-based PPG estimates pulse wave arrival time, which is affected by blood pressure, skin tone, motion, and ambient light. That noise corrupts RMSSD calculations.
Reliable vagal tone measurement
RMSSD is calculated from successive RR interval differences. Even small timing errors compound. A few milliseconds of jitter from PPG estimation can inflate or suppress RMSSD readings significantly. Chest straps provide the clean signal needed for meaningful session-level analysis.
Real-time requires real data
HRV biofeedback relies on immediate, accurate feedback to guide breathing adjustments. Camera PPG introduces latency and smoothing that defeats the purpose of real-time training. Chest straps deliver data fast enough to track your heart rhythm as it responds to each breath.
Gold standard for HRV studies
The published HRV biofeedback literature (Lehrer, Vaschillo, Gevirtz) uses ECG-derived RR intervals, not camera PPG. Respirix follows the same measurement standard so your training data is comparable to what researchers actually measure.
Peer-reviewed references
The published research underpinning each protocol.
HRV & Autonomic Physiology
- Shaffer, F., & Ginsberg, J. P. (2017). An overview of heart rate variability metrics and norms. Frontiers in Public Health, 5, 258.
- Thayer, J. F., & Lane, R. D. (2000). A model of neurovisceral integration in emotion regulation and dysregulation. Journal of Affective Disorders, 61(3), 201–216.
- Thayer, J. F., et al. (2012). A meta-analysis of heart rate variability and neuroimaging studies. Neuroscience & Biobehavioral Reviews, 36(2), 747–756.
Resonance Frequency & HRV Biofeedback
- Lehrer, P. M., Vaschillo, E., & Vaschillo, B. (2000). Resonant frequency biofeedback training to increase cardiac variability. Applied Psychophysiology and Biofeedback, 25(3), 177–191.
- Vaschillo, E., Vaschillo, B., & Lehrer, P. (2006). Characteristics of resonance in heart rate variability. Applied Psychophysiology and Biofeedback, 31, 129–142.
- Lehrer, P. M., et al. (2020). Heart rate variability biofeedback improves emotional and physical health and performance: A systematic review and meta-analysis. Applied Psychophysiology and Biofeedback, 45(3), 109–129.
Slow Breathing & Vagal Activation
- Zaccaro, A., et al. (2018). How breath-control can change your life: A systematic review. Frontiers in Human Neuroscience, 12, 353.
- Russo, M. A., Santarelli, D. M., & O'Rourke, D. (2017). The physiological effects of slow breathing in the healthy human. Breathe, 13(4), 298–309.
Baroreflex Modulation
- Bernardi, L., et al. (2002). Slow breathing increases arterial baroreflex sensitivity in patients with chronic heart failure. Circulation, 105(2), 143–145.
Clinical Applications
- Goessl, V. C., Curtiss, J. E., & Hofmann, S. G. (2017). The effect of heart rate variability biofeedback training on stress and anxiety. Psychological Medicine, 47(15), 2578–2586.
- Laborde, S., Mosley, E., & Thayer, J. F. (2017). Heart rate variability and cardiac vagal tone in psychophysiological research. Frontiers in Psychology, 8, 213.
- Lehrer, P., & Gevirtz, R. (2014). Heart rate variability biofeedback: how and why does it work? Frontiers in Psychology, 5, 756.